A Wall Street Journal headline caught my eye, "Obesity Fuels Custody Fights." It noted that childhood obesity is frequently being used by one parent or the other as grounds for custody changes with accusations concerning poor diets and lack of exercise flying back and forth.
That led me to a July 13, 201 article in The Journal of the American Medical Association (henceforth JAMA), "State Intervention in Life-Threatening Childhood Obesity."
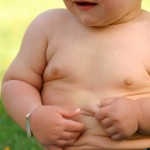
We're not talking about mildly overweight kids here; in 2009 a 555-pound fourteen-yer-old boy, living in one of the southeastern states, was taken by court order from his mother and placed into foster care. She in turn was charged with criminal neglect as the Department of Social Services for that state felt they must intervene or the boy would be at considerable risk for major obesity-related problems, especially diabetes type 2. I found a photo online of the boy and my jaw dropped.
The JAMA article notes "even relatively mild parenting deficiencies" can contribute to a child's weight problems: having junk food in the home, frequently taking the kids to fast food restaurants, failing to model an active lifestyle.The CDC estimates `17% of America's kids and teens are obese (we're not just talking mildly overweight); that's 12.5 million kids at risk. The two Boston authors who wrote in JAMA quote a study showing 2 million of those obese kids are grossly obese with a BMI at or beyond the 99th percentile for their age (a very small percentage of those grossly obese kids, it turns out, may have a genetic abnormality; in those rare cases, the parents aren't to blame).
What can we do about this horrendous problem? Well, there are a variety of "bariatric" operations available in pediatric surgery programs; in dire cases state legal action may be
necessary. But I liked what I saw the other day walking Yoda, our nine-year-old Tibetan terrier, on his morning constitutional (he gets an evening walk as well, which means either my wife or I or both get some extra exercise).
We came near the elementary school near us and there was a long line of kids, punctuated by an occasional teacher, running past. We stopped to watch, realized these were kindergarden and/or first grade kids, and finally had an opportunity to ask one of the teachers what was going on.
"It's a new program we've started in the Poudre School District," she said. "We keep the kids moving for thirty minutes. They can run and most do, or twirl around and walk the field next to the school, but they've got to keep moving."
The conclusion in the JAMA article was stark, but offered a road to resolution. The authors noted, "An increasing proportion of US children are so severely obese as to be at immediate risk for life-threatening complication including type 2 diabetes." They mentioned the pediatric weight loss surgical programs and state protective services, but finished with our need to decrease the need for those options through beefing up the social infrastructure and policies to improve both kids' diets and guide them toward more physical activity.
Those solutions may work.