In a previous post I mentioned former neighbors whose two boys had to run around outside for an hour a day (and they did spend most of that hour literally running), before they got any "screen time." I thought that was admirable and noted both kids were slender.
Now I found an article in the February 15, 2102 issue of JAMA that confirms the wisdom of the approach my friends took toward this issue. A sextet of authors from the UK, Norway, Sweden and Canada published results for the International Children's Accelerometry Database Collaborators (ICAD).
First I had to make sure what accelerometry meant in this context. The dictionary definition was only somewhat useful. It obviously refers to a gadget for measuring acceleration, but when I returned to a prior study of 1,862 British children aged 9 or 10 published in 2009 in the American Journal of Clinical Nutrition, I learned it's a very expensive and sophisticated gadget. My wife has a step counter that our local hospital seniors' organization, the Aspen Club, gave her free. The device used in the large-scale research project, sold by a Florida firm, does lots more than just count steps. Among other thing it also monitors how much energy you expend and what your activity intensity has been. Of course the current model I found online costs $1,249, but there is a volume discount.
That earlier study concluded we need to get our youngsters really moving in order to "curb the growing obesity epidemic."
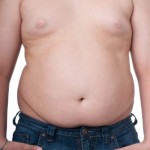
The current paper offers a more nuanced viewpoint. It has a daunting title: "Moderate to Vigorous Physical Activity and Sedentary Time and Cardiometabolic Risk Factors in Children and Adolescents." The study looked at exercise levels and screen time in over 20,000 kids ages 4 to 18. Overall those who got more exercise improved all the risk factors measured: waist size, blood pressure, insulin levels, triglycerides and HDL cholesterol.
Once levels of physical activity were factored in, sedentary time seemed relatively unimportant. But a smaller group, 6413 kids, was followed for a little over two years and neither screen time nor exercise seemed important in changes in waist size, while kids who, at the start of the various studies, had bigger bellies, also had them later. I'd bet most of those were quite TV-addicted, since the paper warns that activity (or lack of activity actually) is often a clue to snacking and soft drinks.
I may show the short form of this paper to the principal of the nearby grade school I've mentioned previously. All those kids, starting in kindergarden, have a one-hour exercise period mostly spent running. I think it's a school-district-wide program and just confirms what to me is common sense.
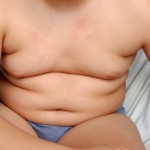
Lots of our youngsters are spending their days sitting in front of a screen of some sort instead of playing active games outdoors. Even in the age group followed in the recent article, a quarter of the kids were at least overweight; 7% were already obese. The average time for active play was a half an hour a day and the average for screen time was close to six hours a day.
I doubt we can totally reverse those numbers, but it's a good idea.